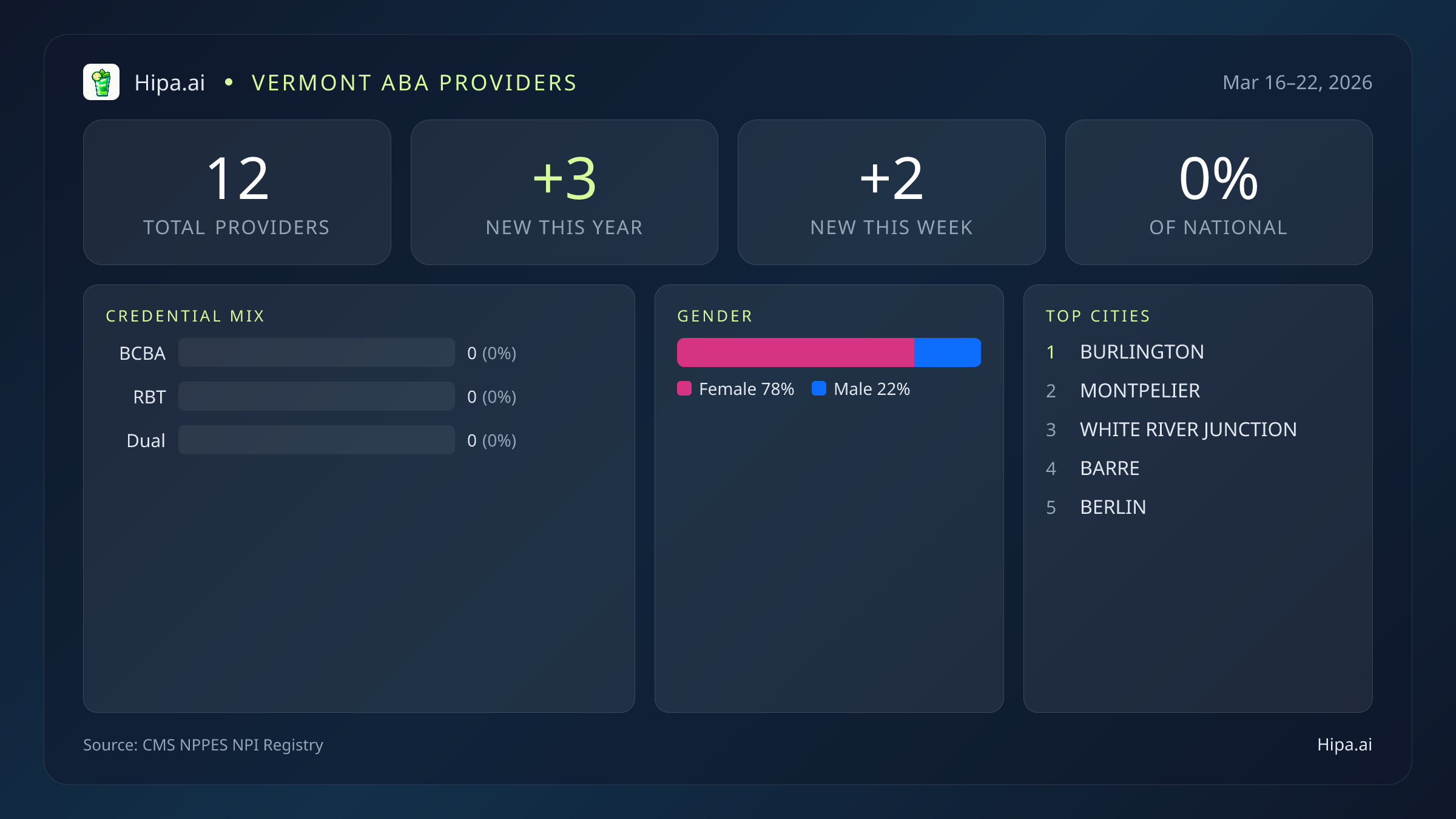
Vermont's behavioral health provider registry contains 12 total providers as of this week's CMS update, with 1 new entrant joining the state's roster. Year-to-date, 3 new providers have registered, suggesting modest but steady workforce growth in a state where ABA infrastructure remains sparse. The state's provider base breaks down into 9 individuals and 3 organizations, a split typical of smaller markets where independent practitioners and small clinics coexist.
Vermont's credential composition reveals a critical gap: there are zero BCBAs, zero RBTs, and zero dual BCBA-RBTs in the registry. Instead, the state's behavioral health workforce is anchored by 4 providers holding master's degrees (MA), 1 licensed clinical social worker, 1 master's in science, and 1 non-clinical therapist. This absence of board-certified behavior analysts signals that Vermont either sources ABA supervision through out-of-state entities or relies on non-ABA behavioral credentials to deliver services. The lack of RBTs—critical frontline technicians who execute treatment plans under BCBA supervision—underscores Vermont's dependence on external talent or alternative service models.
The workforce skews female: 7 female providers (78%) compared to 2 male providers (22%). Providers cluster in five cities—Burlington, Montpelier, White River Junction, Barre, and Berlin—concentrating access in the state's urban and larger towns. Vermont's reliance on non-ABA credentials and absence of certified analysts suggests limited direct ABA availability, likely pushing families toward interstate telehealth or satellite clinic models operated by PE-backed chains serving the broader Northeast region.